|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|
Your Health
Dentists
Doctors
General
Lifestyle
Tooth Decay
|
* Dr. Kugel is Professor and Assistant Dean for Research,
School of Dental Medicine, Tufts University, Boston, Massachusetts, USA ** Dr. García-Godoy is Professor and Director, Clinical Materials Research, Department of Restorative Dentistry, University of Texas Health Science Center at San Antonio, Texas, USA.
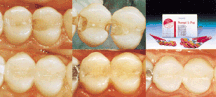
Esthetic direct alternatives to amalgam restorations include glass-ionomers, resin-modified glass-ionomers, compomers and composite restorations. Marked changes in the use of restorative materials have occurred during the past 10 to 20 years1-5 and esthetic considerations are growing in importance for the restoration of posterior teeth.6 Alleged adverse health effects and environmental concerns due to the release of mercury launched controversial discussions about the continued use of amalgam as a contemporary restorative material.7,8 In recent years, development and interest in esthetic dentistry has dramatically increased. This is evident from dental journals publications. Many of the articles and an increasing number of entire journals are devoted to this topic. Along with the journals comes an avalanche of advertisements with products claiming to be the new breakthrough in esthetic restorative dentistry although many times there is nt enough clinical evidence to support their use. The patient population is not immune from this onslaught. They read about bleaching, lasers and metal-free dentistry while standing in line at the supermarket. These same patients are living in a youth oriented society, which places a high value on appearance. Add to this the unsupported fear of mercury in dental amalgams and is it any wonder that the dental professionals are flocking to educational institutes and seminars all across America in search of the esthetic revolution. As amalgam replacements have become a primary focus of dental materials research, the need for improved adhesion has also become an area of major interest. The principles of adhesive dentistry date back to 1955 when Buonocore,9 employing techniques of industrial bonding, suggested that acids could be used as a surface treatment before applying resins. In the late sixties Buonocore et al10 believed that resin tag formation was the cause of adhesion to acid etched enamel. This principle is well accepted today. As we advanced in our understanding of enamel and dentin bonding we also sought to improve those materials we used with our new bonding systems. We marched from our first generation of adhesives, which yielded bond strengths of only 1-3 MPa with poor clinical results, to the present use of fifth and sixth generation systems.11 For example, ESPE's recent entry into the bonding arena is Prompt L-Pop. This is a sixth generation self-etching adhesive system that incorporates the etching of enamel and dentin in one application without a bottle (“bottleless” adhesive).12
Esthetic restorative materials require a bonding procedure in order to be durable and reliable. In order to accomplish this, the bonding system must be biocompatible, bond similarly to both enamel and dentin, have sufficient strength to resist masticatory forces, have mechanical properties close to those of tooth structures, be resistant to degradation in the oral environment and easy to use. The longevity of dental restorations is dependent upon many different factors including materials-, dentist-, and patient-related factors. Main reasons for failure are predominated by the formation of secondary caries, fracture of the bulk of the restoration or of the tooth, marginal deficiencies, and wear. The importance of direct placement esthetic tooth-colored restorative materials is still increasing. Direct composite restorations require a time-consuming and more costly treatment procedure. Our laboratories reported the benefit of using resin-modified glass-ionomers (RMGIs) as liners under posterior composites and amalgams as a way to reduce cervical microleakage13,14 and recurrent caries.15,16 This may be due to their fluoride release.17,18 Glass-ionomers have also been shown to be antibacterial.19 From an esthetic standpoint, glass-ionomers can only be considered as "long-term" provisional restorations in stress-bearing posterior cavities and will not be addressed in this review Direct Adhesive Restorative Materials The availability of fluoride-releasing dental materials have been increasing and the following outline highlights the amount of fluoride release: Fluoride Releasing Restorative Fluoride Release Conventional glass-ionomer High RMGI -->High Smart composite --> High-Med Compomer --> Medium Ceromers --> Low Composite Resin --> Low Packable composite --> Low Flowable composite --> Low Ormocer --> Low Composite Resin Along with improved bonding the clinical performance of direct and indirect restoratives has improved. The most commonly used direct esthetic restorative material is composite resin. The clinical performance of these materials has improved due to developments in wear resistance, color stability, strength, radiopacity and percent cure.20 There are three main factors affecting the properties of composite resins: they are the filler, resin, and interface characteristics. The fillers in composite resins are added to control their handling characteristics, reduce shrinkage, increase strength and decrease abrasive wear. The fillers used include:
One of the major improvements in composite resin has resulted from increased filler loading along with varying its distribution, size, shape and composition.
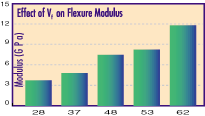
The microfilled composite resin direct restoratives are highly polishable but are subject to increased marginal breakdown.21 Most of the mini-filled composites have a small amount of amorphous silica added to the monomer to improve the handling characteristics. Midifilled composite resins employ zirconium silicate, strontium, or barium fillers and they have an average particle size of 1-3 µm (Table 1). Along with particle size, one must be concerned with filler content. Filler content is the quantity of filler in a composite. It has been demonstrated that filler volume and filler load correlate with the strength of the composite resin. Increased filler volume results in an increase in fracture, toughness (Figure 2), along with an increased flexure modulus22 (Figure 2). The wear of composite restorations depends on filler particle size, interparticle spacing, and filler loading.23 There is reduced wear with smaller particles due to less plucking and therefore fewer voids. Smaller interparticle spacing allows for matrix protection by having the matrix areas smaller than the abrasive particles.
The filler particles of composite resins are silanated in order for the hydrophilic filler to bond to the hydrophobic resin matrix. The importance of silanation is significant. Good silanation will result in a stable composite resin that is resistant to wear with a homogenous composition.24 The matrix of most composite resins is a mixture of di-functional monomers containing Bis-GMA, TEGDMA, or UDMA in some combination. More recent materials such as the ormorcers (organically modified ceramic) employ multi-functional methacrylates. Flowable Composite Resin Also included in the category of composite resins are the flowable composite resins. These resins have lower filler volumes than the conventional direct composite resin restorative materials. As a result of this lower filler volume, these materials have a decreased viscosity, which makes them a good choice as a pit and fissure restorative. However they also have increased shrinkage and increased wear along with decreased strength. They have been recommended as a class V restorative or as a liner under posterior composites. In vitro evidence does not support their use as a liner in order to reduce microleakage.25 Recent Composite Resin Technologies
Compomers Compomers are defined as polyacid-modified resins. These materials are basically light-cured, low fluoride releasing composite resins. The difference between compomers and composites is that the compomers monomers contain acidic functional groups that can participate in an acid/base glass ionomer reaction following polymerization of the resin molecule. The term compomers is the result of the hybridization of the words composite and glass ionomer. However, they are not glass-ionomer materials. A true glass-ionomer must be a two-component system or else the acid/base reaction would take place immediately.24 Conventional glass-ionomers must be mixed just prior to use. With the compomers, there is a single component system which cannot contain any water in order to prevent a premature glass-ionomer reaction. A resin polymerization takes place with the compomers after the material has set completely. The glass-ionomer reaction may then occur in the presence of water. Water is a necessary medium for the acid/base reaction. In the presence of water from the oral cavity, the acid functional groups, which are attached to the monomer units, and have now become part of the polymerized material are able to react with the base (glass) to stimulate the glass ionomer reaction. Fluoride is released as a result of this reaction. The level of fluoride release from the compomers is significantly lower than what is seen for conventional glass-ionomers or RMGIs.26 When they were introduced, acid etching was not required by the manufacturers. This was seen as an advantage over the use of composites along with the suggested fluoride release. It was subsequently demonstrated that the use of an acid etched procedure significantly improves both the retention and marginal leakage of the compomers.27-29 In summary, compomers:
Packable Composites As the dental profession searched for an amalgam substitute it found limitations in the composite materials on the market. These limitations included: resistance to wear, fracture of the restoration within the body and at the margins, marginal leakage due to polymerization shrinkage and the technique sensitivity including the ability to obtain adequate proximal contact in the final restoration. Packable or "condensable" composites have recently been introduced to the profession as an amalgam substitute. They contain a higher filler load as well as filler distribution. This results in a stiffer consistency than hybrid composites. These changes in the properties of the packable composites result in improved handling characteristics, at least as seen by the manufacturers of these products. The major advantage to these materials is that they make it easier to establish inter-proximal contacts while placing class II restorations. Some of these materials also claim that they may be cured in bulk. Recent studies have indicated that some of the packable composites claiming bulk fill to 5 mm depth fall short of these claims.
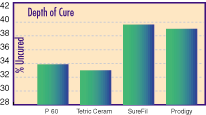
One study using a halogen light demonstrated at a 40-second cure that the uncured values are 39.08% for Prodigy, and 39.61% for Surefil, both of which claim to be bulk fill materials. The results for the two materials, which recommend incremental cure, were 33.76% for P60 and 33.19% for Tetric Ceram30 (Figure 4). Bingham JDR 1518A:2000 Ceromers The term ceromer stands for Ceramic Optimized Polymer and was introduced by Ivoclar to describe their composite Tetric Ceram. This material consists of a paste containing barium glass (< 1 µm), spheroidal mixed oxide, ytterbium trifluoride, and silicon dioxide (57 vol%) in dimethacrylate monomers (Bis-GMA and urethane dimethacrylate. They are set by a polymerization of C=C of the methacrylate. They must be bonded to tooth structure. The properties of the ceromers are identical to those of composites and they exhibit fluoride release lower than conventional glass-ionomers or compomers. Ormocers Ormorcer is the acronym for Organically Modified Ceramics. This class of material represents a novel inorganic-organic copolymer in the formulation that allows for modification of its mechanical parameters. The inorganic-organic copolymers are synthesized from multi-functional urethane- and thioether(meth)acrylate alkoxysilanes as sol-gel precursors. Alkoxysilyl groups of the silane permit the formation of an inorganic Si-O-Si network by hydrolysis and poly-condensation reactions. The methacrylate groups are available for photochemical polymerization.3,31 The filler particles are 1-1.5 µm in size and the material is 77% filler weight and 61% filler volume. "Smart" Composites This class of composites was introduced as the product Ariston pHc in 1998. Ariston pHc is an ion-releasing composite material. It releases fluoride, hydroxyl, and calcium ions as the pH drops in the area immediately adjacent to the restorative material. The drop in pH values is the result of active plaque which results in a corresponding increase in the release of functional ions.3 Smart composites work based on the newly developed alkaline glass filler which will reduce secondary caries formation at the margin of a restoration by inhibiting bacterial growth. This results in a reduced demineralization and a buffering of the acid produced by caries forming microorganisms.31 The paste consists of Ba, Al, and F silicate glass filler (1 µm) with ytterbium trifluoride, silicon dioxide and alkaline Ca silicate glass (1.6 µm) in dimethacrylate monomers: it is filled 80% by weight and 60% by volume. The use of an adhesive to tooth is not recommended. However dentin should be sealed to reduce sensitivity. The fluoride release from this material is claimed by the manufacturer to be lower than conventional glass-ionomers but more than that of compomers. Indirect Adhesive Restoratives In an effort to address the disadvantages of the direct adhesive restoratives such as technique sensitivity, anatomic form, polymerization shrinkage, wear and interproximal contacts, the indirect composite resins were introduced. These materials were also seen as having advantages over PFM and all ceramic restorations. PFM restorations require a metal substructure, although reliable and time-tested, they are often considered as esthetic as the all-ceramic or indirect composite restorations. It is difficult to obtain the translucency seen in natural teeth when using a metal substructure. While the all-ceramic restorations are more translucent than PFM, they have other problems, such as abrasion of the natural dentition and they are not easily repaired. First Generation The first generation of the composite–based indirect adhesive restoratives were introduced in the early 1980’s. These included Visio-Gem (ESPE) and Dentacolor (Kulzer) followed in 1987 by Concept (Ivoclar). These materials were developed in an effort to overcome the polymerization shrinkage and accelerated wear experienced with the direct adhesive restorative materials. These new materials offered the advantages of chairside repair, esthetics, improved anatomy and interproximal contact along with ease of fabrication. However, this first generation of materials suffered from low flexural strength, low modulus of elasticity and low resistance to wear abrasion. These poor physical properties were the result of low filler load and high matrix load. Second Generation It was not until the mid-1990’s that the second generation of indirect composite restorative were introduced. These new materials included Artglass (Heraeus-Kulzer), BelleGlass HP (Kerr), Targis (Ivoclar), Colombus (Cendres et Mataux) and more recently, Sinfony (ESPE).
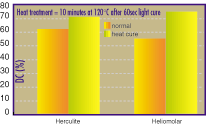
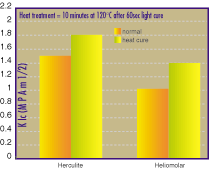
The effect of heat curing these newer composite materials
on the degrees of conversion was demonstrated by Ferracane and Condon in
199232 (Figure 5). They demonstrated that heat treatment, in
addition to a 60-second light cure, will increase the degree of
conversion. This increase in degree of conversion will improve the
fracture toughness of the indirect composite materials (Figure 6).
This second generation of materials incorporated ceramic
fillers with mean particle sizes of less than 1 µm of smaller diameter,
silanized and with a narrow distribution. The filler is commonly barium
silica. They have a high filler load (70-80% by weight and 50-60% by
volume) and they have a lower resin content (approximately 33% resin
matrix by volume.) As discussed earlier, the filler volume and filler load
correlate with the strength of a composite resin.22 The higher
filler load will help reduce the polymerization shrinkage, while it
increases the modulus of elasticity.
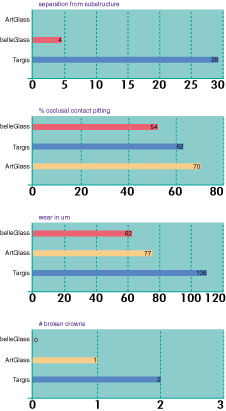
Wear data from the manufacturer is reported as being quite low. BelleGlass is reported by the manufacturer as having wear of 1.2 µm for 1 year. The CRA in 1998 reported their findings as being quite different. Belleglass was shown to wear at 62 µm per year, Targis, 106 µm, and Artglass, 77 µm (Figure 7). In an attempt to expand the use of these materials, Kulzer attempted to bond their polymer glass, Artglass to a metal substructure. The results were less than satisfactory. Depew and Sorensen33 demonstrated that of 49 units placed, at year 1, 32% failed and at year 2, they had a 39% failure rate. Ninety percent of these failures occurred by the composite veneer debonding from the metal. They also reported mean maximum wear depth of 113 µm (SD56-480 µm). Their conclusion was that Artglass to metal is unreliable with high failure rates and wear. More recently ESPE has entered this arena with their product, Sinfony. This composed of 48% monomers, 1% initiator, 40% ultrafine glass, 5% pyr. silica acid, 5% glass-ionomer and 1% silane. This material shows promise but needs further evaluation. Fiber-Reinforced Substructure This second generation of indirect composite resins may be combined with fiber-reinforced substructure. This technology was used for periodontal splinting as well as temporary bridge reinforcement to its introduction as a reinforcement for indirect composite restoratives.34 The fibers used for this purpose are composed of carbon Kevlar, polyethylene and glass fibers (Table 2).
These fibers may be preimpregnated with resin. The preimpregnated fibers are silanized and coated with resin. This will provide a cohesive bond to the resin matrix. Indications for indirect composite restoratives are: - Metal free dentistry - Esthetics - Decreased wear of opposing dentition (as compared to porcelain) - Conservative tooth preparation35 Contraindications include: -Bruxism/clench -Opposing porcelain -Long span fixed partial dentures -High caries rate -Difficult moisture control during adhesion The CRA Newsletter reported in 1998 surface degradation of the initial polish with significant wear rates. They also noted high levels of post insertion sensitivity. Finally, delamination from the fiber reinforcing substructure due to layering techniques used during the fabrication process have been reported.36,37 Ceramic Adhesive Restorative This group of materials include the press ceramics such as IPS-Empress, OPC, Finesse, Creepers and VitaPress along with the reinforced core materials such as In-Ceram and Procera. These offer improved esthetics and strength but they are more difficult to fabricate and they cannot be repaired. The additional issue arises that the reinforced core materials cannot be bonded. In addition to the pressed and reinforced ceramics, there are the ceramic adhesive restoratives that are ground from preformed blocks. These are machined by use of computer-aided design/computer-aided manufacturing (CAD/CAM) or by a copy milling unit. Conclusions There is a plethora of direct and indirect adhesive restorative materials on the market. The average dentist is often overwhelmed by the choices. Many times one material offers little advantage over another. However, as the push for improved esthetics continues to grow, so will our list of materials. So long as there is a market, the manufacturer will introduce new products. As dentists we must not only rely on the materials but on our own ability to treatment plan and diagnose based on a multifactorial situation. We must be careful in our preparation, design, communication with a skilled laboratory technician and be meticulous in our bonding techniques. Failures in dentistry are frequently blamed on the materials. In reality, “user error” is often the culprit. Interpreting the research data and understanding our options based on the patients’ caries risk status are the first steps toward success. References
|
Other Reviews:
Rotary Endodontic Instrumentation
Direct & Indirect Esthetic Adhesive Restorative Materials
Early and Immediate Loading of Implants
Lasers in Root canal treatment and Endodontics
Abfractions? How they are important in Restorative Dentistry
Latest Research On Dental Pain
More Articles
Restoration of endodontic teeth
Options for esthetic restorations
Teeth Whitening Facts and Myths
Fiber reinforced composites in dentistry
Changing concepts in Class I and II cavity preparation
Curing lights for composite resins
Caries Prevention in Children - The Indian Challenge
Mouth Rinsing before dental procedures.
Shade selection and Management
Obstructive Sleep Apnea- Do you know about it?
Genetically modified bacteria may prevent cavities - Put you out of Business?
A primer on all composite class materials
Immediate and Early loading of Implants
Placement of gingival restorative margins
Bonding for the New Millennium
Access Cavity Preparation - Molars
New cavity-fighting agent shows promise
Tooth Loss Linked to Pancreatic Cancer in Smokers
2-min brush helps achieve cleaner teeth: Study
Gum disease raises death risk in diabetics: study
Brushing Right After Drinking Soda may Harm Teeth
Benefits of Pre-procedural mouth rinsing?
To Bond Or not to Bond Amalgam
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||